Blog
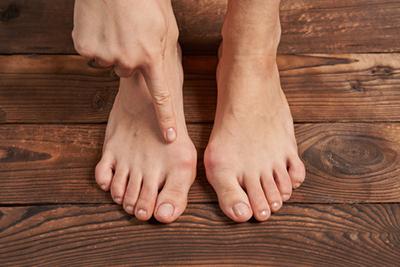
Preventing and Managing Bunions: What You Need To Know
- posted: Apr. 11, 2024
Bunions are bony bumps that protrude and develop at your big toe's base joint. Bunions typically grow slowly and take time to develop; however, they ultimately cause pain and an Read More
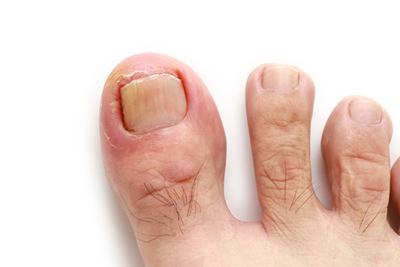
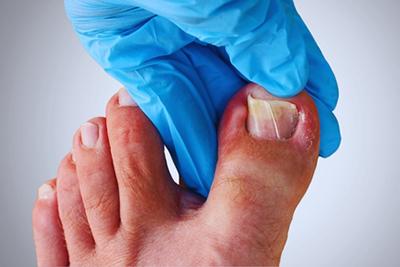
Symptoms of an Ingrown Toenail
- posted: Apr. 01, 2024
Ingrown toenails are painful and ugly. They can make it difficult to put on shoes, to stand, and to walk without pain. An ingrown toenail can decrease your mobility. Your Read More
A Guide to Preventing Ingrown Toenails
- posted: Mar. 21, 2024
Onychocryptosis – or an ingrown toenail refers to a common foot ailment that happens when the edge of one of your toenails pierces the surrounding skin, creating pain and other Read More
Managing Your Heel Pain
- posted: Mar. 01, 2024
Your heels are nature’s shock absorbers, providing a cushion for standing, walking, and running. If you’ve ever experienced heel pain, you already know how it can impact your life. The Read More
What You Need To Know About Ingrown Toenails
- posted: Feb. 01, 2024
Ingrown toenails can happen to anyone. If you have an ingrown toenail, chances are it’s difficult to put on shoes and want to walk around. Your podiatrist can help with Read More
Orthotics and Their Role in Foot Health: Custom Solutions for Various Conditions
- posted: Jan. 01, 2024
Do you have foot problems? Do your feet hurt all the time? If so, you need to discover the benefits of orthotics. This common treatment, available from your podiatrist, can Read More
Common Foot and Ankle Injuries in Athletes
- posted: Dec. 06, 2023
Regional Foot and Ankle Specialists and our team of specialists can help with a variety of issues that could impact athletes. For example, we can help you handle foot and Read More
Preventing Foot Injuries: Tips for Proper Foot Care and Injury Avoidance
- posted: Dec. 01, 2023
If you experience a foot injury, it can dramatically impact your quality of life. Depending on the injury, foot injuries can lead to loss of mobility, inability to drive, lost Read More
The Benefits Of Orthotics
- posted: Nov. 01, 2023
Orthotics are custom-made shoe inserts or insoles designed to support and correct irregularities in foot function. They aim to alleviate various foot and ankle conditions, providing relief and improved mobility. Read More
The Importance of Diabetic Care
- posted: Oct. 01, 2023
When you’re dealing with diabetes, it’s important that you’re getting all the care that you need to ensure every part of your body. One big issue is making sure that Read More
Taking Care of Your Feet: The Importance of Podiatric Health
- posted: Sep. 22, 2023
Podiatry is a specialized branch of healthcare focused on diagnosing, preventing, and treating conditions affecting the feet and ankles. If you experience discomfort, pain, or concerns about your lower extremities, Read More
Bunion Treatment Options
- posted: Sep. 01, 2023
If you have a bunion, you are not alone. A bunion is one of the most common, and painful foot problems your podiatrist can treat. What You Need To Know About Read More
How You Can Prevent Plantar Fasciitis Symptoms
- posted: Aug. 23, 2023
Plantar fasciitis affects many Pennsauken, and Turnersville, NJ, residents. This common foot condition is a very frustrating and can cause pain and mobility problems. These symptoms can be prevented if Read More
Foot Health for Children
- posted: Aug. 01, 2023
When you think about taking care of your child, you may not be thinking about taking care of your child’s feet. The truth is, foot health for children is important, Read More
Diabetes and Foot Care: Tips for Maintaining Healthy Feet
- posted: Jul. 01, 2023
Diabetes is a serious disease, affecting many of the major systems of your body, including your immune, circulatory, and nervous systems. The effects of diabetes are especially evident in your Read More
What You Need To Know About Taking Care of Your Feet
- posted: Jun. 01, 2023
Running and staying active are healthy choices for your body and mind. The health of your feet is very important if you want to stay active. Your podiatrist can help Read More
This website includes materials that are protected by copyright, or other proprietary rights. Transmission or reproduction of protected items beyond that allowed by fair use, as defined in the copyright laws, requires the written permission of the copyright owners.